What is Nail Pitting?
Nail pitting is a common disorder affecting the surface of fingernails or toenails. It presents as small, round depressions on the nail plate. Often, the pits look like tiny punctures or dots. Sometimes these dots may form linear patterns. Nail pitting can range in severity. Some people notice only a few pits, while others have many pits on several nails. The number and size of the pits can vary over time. This condition can be a standalone issue or a sign of other health conditions. Nail pitting may be an issue for appearance to some, but for others, it could indicate deeper health concerns. It’s important to understand what causes nail pitting and when to seek medical advice. Appropriate treatments and home practices can improve the look and health of your nails. Recognizing nail pitting early can lead to better outcomes with proper care.
Common Causes of Nail Pitting
Nail pitting often stems from certain diseases or conditions. Sometimes it appears without clear reason. One major cause is psoriasis, an autoimmune skin condition. In addition, eczema, another skin issue, can lead to nail pitting. Alopecia areata, which causes hair loss, may also affect the nails. Repeated nail trauma or injury is another common factor. This includes frequent nail biting or picking. Some skin conditions linked to nail pitting are genetics-based. This means they can pass down in families. Less commonly, nail pitting can result from certain infections. Fungal infections in nails often change their appearance. Nutritional deficiencies, especially low zinc, may cause pitting. The use of harsh nail products can contribute too. To understand the precise cause, a healthcare professional’s input is vital. They can link nail changes to other symptoms you may have.
Nail Pitting and Psoriasis: What’s the Connection?

Nail pitting often signals underlying health concerns. One well-known link is with psoriasis. Psoriasis is an autoimmune disease causing skin cells to multiply rapidly. This leads to thick, red patches and silvery scales on the skin. Around 50% of individuals with psoriasis experience nail changes. This includes nail pitting.
The reason for this connection lies in the disease mechanism. Psoriasis can affect the nail matrix. This is where new nail cells come from. When psoriasis affects this area, it can disrupt nail growth. The result is the development of pits on the nail’s surface.
Moreover, psoriatic nail disease comes in various forms. Besides pitting, nails may become discolored or detach from the nail bed. Understanding the severity of nail psoriasis is important. It can guide treatment choices. Treatments aim to reduce symptoms and improve nail appearance. In some cases, treating the underlying psoriasis reduces nail pitting.
Anyone seeing changes in their nails with known psoriasis should speak to a doctor. The doctor may alter the treatment plan or suggest specialized care for nails. It is key to address both skin and nail symptoms together. Combining treatments can lead to better control over the condition. Monitoring the health of your nails can signal if psoriasis treatments are effective.
Other Health Conditions Associated with Nail Pitting
While nail pitting is most commonly linked to psoriasis, it is not the sole condition that can lead to this nail change. Several other health issues play a role in creating these small, indentations in the nails. It’s essential to consider these conditions, as their treatment may differ from those applied in psoriasis cases.
- Eczema: This skin disorder, characterized by itchy and inflamed skin, can also affect the nails.
- Alopecia Areata: Not only does this condition result in hair loss, but it can alter nail texture, leading to pitting.
- Rheumatoid Arthritis: This autoimmune disorder affects joints but can show up in nails as pitting or abnormalities.
- Lichen Planus: An inflammatory condition affecting skin and mucous membranes, including the nail bed, which can cause pitting.
- Sarcoidosis: This growth of inflammatory cells can occasionally manifest in the nails as pits or other irregularities.
Individuals with nail pitting should take the association with these conditions seriously. Early diagnosis can open up more effective treatment avenues. As always, tracking changes and consulting with a healthcare provider is most critical to ensure a correct diagnosis and optimal care plan. Any persistent changes in nail health merit a professional evaluation to rule out or confirm the association with these conditions. Remember, nail health often reflects overall body health, so staying vigilant about nail changes can be a window into diagnosing other health issues.
Diagnosing Nail Pitting
When faced with nail pitting, proper diagnosis is crucial to pinpoint the underlying cause. The process involves a thorough examination by a healthcare provider. They will look closely at your nails for patterns and severity of the pits. The doctor may ask about your personal and family medical history. They want to know if there are any known skin conditions, such as psoriasis or eczema.
To confirm a diagnosis, the doctor might conduct several tests. These can include nail clippings, which are sent to a lab to check for fungal infections. Blood tests are also common to look for signs of autoimmune disorders, like rheumatoid arthritis or psoriasis. In some cases, a small biopsy of the nail bed may be necessary. This helps to rule out other skin conditions.
The findings from these efforts guide the next steps. For instance, if psoriasis is the cause, your doctor will focus on treating that condition. This approach could reduce or eliminate nail pitting. Should the tests reveal a fungal infection, antifungal treatments would be prescribed.
It’s important not to self-diagnose nail pitting. Over-the-counter treatments may not address the actual problem. They could even make things worse. If you notice any changes in your nails, it is best to consult with a healthcare professional. They have the right tools and knowledge to provide an accurate diagnosis and recommend effective treatments.
Treatment Options for Nail Pitting

Treating nail pitting requires a targeted approach, depending on the underlying cause. Here are the main treatment options:
- Topical Treatments: Doctors often prescribe creams or ointments. These can include corticosteroids to reduce inflammation.
- Light Therapy: For cases related to psoriasis, UV light therapy can be effective. It slows down cell growth and eases skin symptoms.
- Medications: Immunosuppressant drugs may help with autoimmune-related nail pitting.
- Nail Care Practices: Keeping nails trimmed and clean avoids further damage. Nail hardeners may strengthen the nails.
- Diet and Nutrition: Proper intake of vitamins and minerals supports nail health. Supplements like zinc might improve nail quality.
Remember to not pick or bite at nails, as this can worsen the pitting. If nails are thickened or difficult to trim, seek professional manicure services that can manage nail care safely. Consult with a healthcare provider before starting any treatment regimen, especially when dealing with autoimmune conditions. Taking the right steps can improve nail health and overall well-being.
Home Remedies and Prevention Tips
While medical treatments for nail pitting are crucial, some home remedies and prevention strategies can also be beneficial. Here are tips to maintain healthy nails and possibly prevent it from occurring or worsening.
- Keep Nails Clean and Dry: Prevent infections by keeping your nails clean and moisture-free. Avoid long soaks in water.
- Moisturize Your Nails: Just like skin, nails need to stay moisturized. Use a gentle cream or oil daily.
- Avoid Nail Damage: Be gentle with your nails. Avoid habits like nail biting or using your nails as tools.
- Wear Gloves: During household chores and while gardening, protect your nails with gloves to prevent damage.
- Stop Using Harsh Nail Products: Avoid nail polish removers with acetone and harsh chemicals that can cause nail pitting.
- Eat a Balanced Diet: A healthy diet rich in vitamins and nutrients supports overall nail health. Focus on foods high in biotin and zinc.
- Reduce Stress: Since stress can trigger conditions like psoriasis, finding ways to manage it can help prevent nail issues.
- Trim Nails Regularly: Keeping nails trimmed will reduce the risk of trauma, potentially preventing the formation of pits.
Implement these simple tips as part of your daily routine for maintaining nail health. Pairing these practices with your doctor’s advice can lead to the best care for your nails. If you have any concerns or if prevention strategies do not help, a doctor’s visit is necessary to explore further action.
When to See a Doctor About Nail Pitting
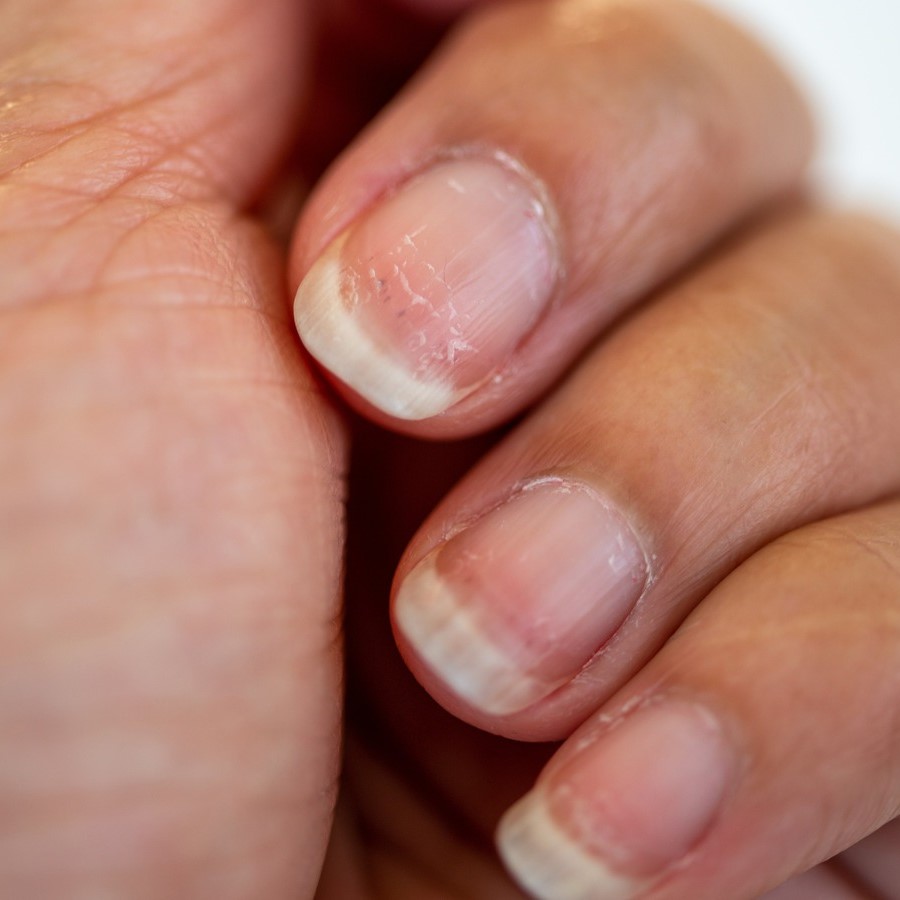
It is generally advisable to consult a healthcare professional if you notice any unusual changes in your nails. Nail pitting, while sometimes benign, can be a sign of underlying health issues that require medical attention. Here are specific instances when you should seek a doctor’s advice:
- Persistent or Worsening Condition: If nail pitting does not improve or worsens, see a doctor.
- Multiple Nails Affected: When several nails are pitted, it might signal something systemic.
- Associated Symptoms: If you experience joint pain, skin rashes, or hair loss, get checked.
- No Clear Cause: When there is no apparent explanation, like an injury, seek medical advice.
- Nail Color or Shape Changes: Changes in color or nail detachment need a professional opinion.
Early intervention can lead to more effective treatments and help prevent potential complications. If nail pitting comes with discomfort or pain, do not delay in consulting a doctor. Remember, your nails can provide insight into your overall health, so taking changes seriously is important. Tracking your nail health and discussing any irregularities with a physician ensures that any concerns are addressed promptly and appropriately.